Dial Fellows
A promising approach to community-driven care amid a pandemic
Dr. Sriram Shamasunder and his organization, HEAL Initiative, stood in solidarity with Navajo healthcare workers as they fought a COVID outbreak through the spring and summer.
This past summer, when the Navajo Nation was the site of one of the country’s worst coronavirus outbreaks, Dr. Sriram Shamasunder was at Chinle Comprehensive Health Care Facility in Arizona, caring for a Navajo elder in the respiratory care unit. When he was young, the patient had worked in the uranium mines on Navajo land, and he had spent decades drinking water contaminated with the radioactive element. He had poor baseline lung function, and now he had COVID-19. His family could not be there to comfort him. He was isolated and scared.
COVID-19’s novelty — and the lack of proven medical interventions to use against it — forced caregivers to consider non-clinical aspects of care, and to approach clinical encounters with what Shamasunder calls “full presence.” Shamasunder is a published poet, and his doctor’s sense of care is also a poet’s sense of language: a doctor can choose a series of interventions, and a poet, a series of words — prescriptions, positions, verbs, nouns, supplemental oxygen — but the ultimate effect is ineffable, determined by empathy, relationships, and lived experience.
On harried rounds in the overwhelmed medical center, it was very difficult to be fully present. “I was moving fast. I was wearing goggles, a face shield, an N95 mask,” Shamasunder recalls. He couldn’t speak to the miner in his own language, and he wasn’t intimately familiar with the contours of the man’s life on the reservation. There was a gulf between them that Shamasunder, as his doctor, struggled to cross.
But Shamasunder had not come into the room alone. He was accompanied by Navajo nurses from the local community. “They would just lean over in his ear and speak to him in his own language,” Shamasunder says, “‘I won’t let you go.’ ‘I am from your community, and I’m here to stand with you.’ To bridge that gap is just so powerful.”

Signs encourage safety in the Navajo Nation. Photo credit: UCSF
Shamasunder, an Emerson Collective Dial Fellow, was in Navajo Nation with HEAL Initiative, the organization he co-founded. HEAL is a global health equity fellowship that deploys early-career, U.S.-based doctors and nurses to train alongside clinicians from the communities the organization serves. During the pandemic, HEAL has been celebrated for coordinating the arrival of additional medical staff from the University of California, San Francisco — Shamasunder’s and HEAL’s home institution — to assist with care in Navajo communities. In May, per-capita infection rates in the Navajo Nation surpassed those in New York City. But by late summer, Navajo Nation had dramatically bent the curve. HEAL’s thoughtful integration of UCSF clinicians into care teams on the reservation and focus on systemic issues affecting the health of Navajo people were crucial to the efforts.
What made HEAL so effective? It may have had something to do with the way HEAL responds to the problem Shamasunder has spent his entire career thinking about: How can the best care be delivered across the human boundaries of language, culture, gender, and religion that arise in our global community? After the technical training of medical school, can young health professionals be trained in the ineffable part of the practice, in leadership, advocacy, and justice?
How can they learn to show up in their full presence?
Dr. Sri ShamasunderI think there was a question all of us sat with. What does it mean to lead a purposeful, committed life? What does that look like?
In his sophomore year of college at the University of California, Berkeley, Shamasunder enrolled in a class called “Poetry for the People,” taught by the poet June Jordan. Jordan was a contemporary of Toni Morrison and Audre Lorde, and was mentored by Malcolm X and Fannie Lou Hamer. Shamasunder remembers how Jordan’s class was animated by her insistence that one ought to stand alongside those who suffer; to advocate for them; and to put one’s own person on the line in solidarity with them. It was a perspective that transformed her students. “I think there was a question all of us sat with,” Shamasunder says. “What does it mean to lead a purposeful, committed life? What does that look like?”
Shamasunder’s own coming of age had primed him to consider such questions. He grew up north of Los Angeles, in a community composed primarily of the working poor. When Shamasunder was just shy of six years old, his father nearly died from kidney failure. He was saved by years of dialysis, and by the donation of a kidney from Shamasunder’s aunt, who lived in India, a place Shamasunder had visited on family trips and where he observed “deep injustice and inequity.”
While at Berkeley, he attended a talk by Dr. Paul Farmer, the co-founder of the global health organization Partners In Health, and was deeply moved by Farmer’s commitment to the human right to health. As Shamasunder pondered the question of purpose, he thought about Farmer’s program model, and Jordan’s class. He began to think that, as a doctor, he could be especially useful in resource-denied communities. After completing his medical residency, he was hired at UCSF, where he negotiated the ability to split his time among the Bay Area, and international venues. He joined Partners In Health, and worked around the world: Rwanda, India, Haiti, Burundi.
Shamasunder worked in Burundi in his first year out of residency. He thought he’d show up and be instantly effective. Instead he encountered “so much needless death.” Mothers would come in with sick children — who should have been treatable, even in an impoverished, rural setting — and later, he’d watch them strap their dead children to their backs for the journey home. It was a confrontation with the ravaging inequity of health care — an inequity often exacerbated by a colonialist tendency, particularly among American health care institutions, to imagine they could “drop in” to communities for only weeks at a time and succeed in delivering meaningful care.
At the same time, Shamasunder observed that his Burundian colleagues were driven by the same goals as his own — to deliver the best care, to have maximal impact, to be useful — but were equipped with far fewer resources. He began to imagine a way they could bolster one another’s efforts –– a way to better train and support both the medical workers like himself, coming in from the outside, and the medical workers with lifetimes of experience in their communities.
Years later, Shamasunder and a colleague, Dr. Phuoc Le, started HEAL Initiative.
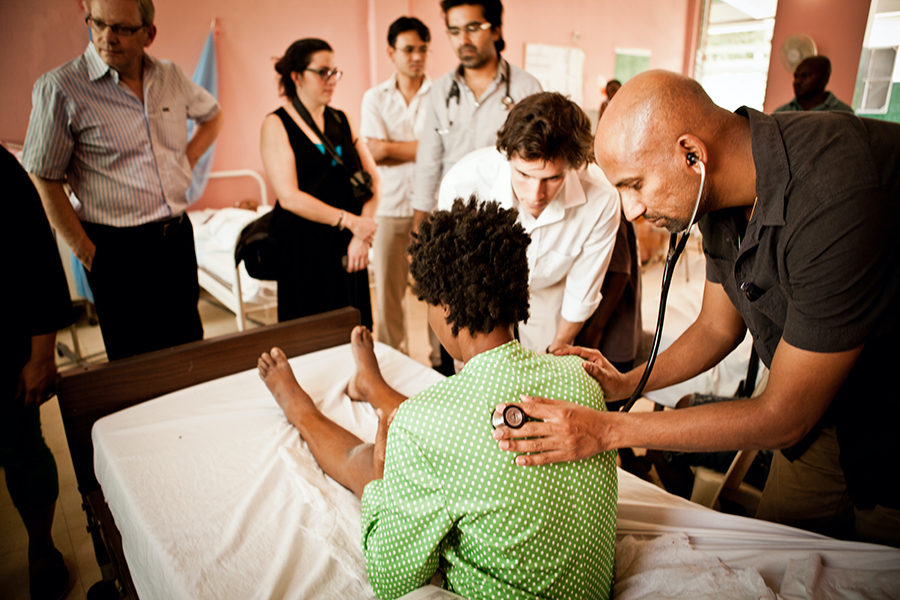
Dr. Shamasunder treating a patient in Haiti. Photo courtesy Sri Shamasunder
HEAL offers two, interdependent fellowships. “Rotating fellows” are U.S.-based physicians and nurses, who spend two years serving in under-resourced locations across America and abroad. “Site fellows” are health professionals drawn from those locations. All fellows train and work together, drawing from one another’s experiences. While the rotating fellows are all young professionals who have recently completed their residencies, the site fellows come from all stages of life. The program’s structure is a bet that the technical aspects and the ineffable qualities of care both flourish in community.
Although partner sites were drawn largely from Shamasunder’s and Le’s experiences in global health, they knew they wanted some grounding in domestic work, too. This is how, in 2014, Shamasunder found himself in the Navajo Nation, discussing the partnerships that would become central to HEAL’s work.
The Navajo Nation clinical sites Shamasunder engaged were interested in the support HEAL could provide, especially since more than a quarter of their positions were vacant. But there was also initially a lack of trust, generated by temp agencies that had performed woefully, and in a larger sense, stemming from chronic disinvestment, broken promises, and broken treaties.
HEAL’s model of prioritizing site fellows, who receive extensive training and mentorship, plus professional development with the option to pursue an advanced degree, allayed some of the community’s fears by illustrating HEAL’s commitment not just to health on the reservation but to elevating Navajo health care workers. At its inception, HEAL had more site fellows drawn from within the Navajo Nation than it had rotating fellows who hailed from outside it.
One early site fellow, Michael Tutt, was a Navajo elder. Shamasunder observed that Tutt was a wonderful presence in the cohort, but was reticent during much of the organization’s programming. Curious, he asked Tutt what had drawn him to the fellowship. “I just wanted to vet you all,” Tutt told him, “because as a Navajo elder, to be a health worker is to be a protector of the people.” Tutt would eventually spend time on HEAL’s steering committee.
The relationships HEAL built were lasting. The infrastructure of care in the community improved. “We were actually working ourselves out of a job,” Shamasunder says.
Then, five years in, COVID-19 erupted.

Sewing PPE in Chinle in the Navajo Nation. Photo credit: UCSF
In May, a disheartening thread of stories about COVID-19 in the Navajo Nation was circulating. Per-capita infection rates soared. Congress had approved $8 billion in coronavirus relief for tribes around the country, but the money did not arrive as committed. It was a cruel echo of the disinvestment that had left the Navajo Nation — an area larger than West Virginia — with just 13 grocery stores and only some 20 ICU beds.
HEAL got the news sooner, because they were already in the community. By early April, Shamasunder knew of the resource crunch: nurse shortages; respiratory care units forced to turn back patients; ICU beds filling up in crucial transfer facilities in Albuquerque and Phoenix, where Navajo clinics and hospitals would send patients with cases too advanced for them to treat.
HEAL began routing its international fellows to the reservation. At the same time, UCSF had sent nurses to New York. As the situation calmed there, Shamasunder suspected he might be able to convince the university to direct resources to the Southwest. He leveraged HEAL’s history in the community to underscore the urgency of the ask. “I made the case that we’re entrenched here, we’re committed here. There’s a COVID surge, and they really are struggling, and we have the relationships and the partnerships to help,” Shamasunder says.
Before the month was out, HEAL had invited more than 25 volunteer health professionals to the reservation. By July, nearly 25 more — and this in addition to the 50 HEAL fellows who live and work permanently in the Navajo Nation. Through its relationships and volunteer training, HEAL was able to seamlessly integrate the volunteers into the provision of care.
“We were just standing toe-to-toe with our fellows,” Shamasunder says. “We actually had trust from those communities. They knew HEAL.” By the end of a long, heartbreaking summer, the Navajo Nation was prevailing over the disease. Patient volumes decreased and lockdowns were eased. The peak of the crisis this summer was over.
Dr. Sri ShamasunderPart of the problem in the world is that the locus of power exists at an institution in San Francisco. That’s not how the world changes.
In the wake of this progress, UCSF is compiling a report on the efforts of HEAL and the volunteers in Navajo Nation. Shamasunder’s own reflections, unsurprisingly, have so far taken the form of notes and sketches of new poems that address the work of the health professionals in their full presence, affirming their spirit of partnership and solidarity. He wants to make sure the opportunity to explore those elements of the summer’s efforts is not overlooked — by the medical community, or by HEAL. The organization’s next five years, he says, are about making sure Navajo fellows shape the work — and so too in India, Haiti, and all of its sites. “Part of the problem in the world is that the locus of power exists at an institution in San Francisco,” he says. “That’s not how the world changes.”
And the world must change. This fall has seen COVID-19 case counts rise around the globe, and the Navajo Nation has not been exempt. In late October, with a surge in New Mexico taking hospitals in Albuquerque beyond their bed capacity, the reservation’s command-control structure re-engaged in planning for case management and potential patient transfers to hospitals all over Arizona and New Mexico. Just this week, after announcing that 34 Navajo communities have “uncontrolled spread” of the disease, the nation’s leadership instituted a three-week lockdown restricting nonessential activities. Shamasunder is trying to coordinate another team of nurses to travel down to Arizona and New Mexico to help. If he is needed, there is no question that he would return to the desert.
As the organization’s profile has risen this year, Shamasunder has been reflecting on HEAL’s work. As a first-year medical resident, he had visited Jordan after she’d had a tough day in the classroom. Her dog jumped on him and tracked dirty paw prints on his shirt, and Jordan insisted that he leave it with her to be washed. She returned it, along with a poem, “It’s Hard to Keep a Clean Shirt Clean,” which is dedicated to him. It reads, in part:
It’s clean.
A clean white shirt
nobody wanted to spoil
or soil
that shirt
much cleaner now but also
not the same
as the first before that shirt
got hit got hurt
not perfect
anymore
just beautiful
This poem, one might say, is about a particular way of thinking about the world and how to be alive in it –– with full presence, and groundedness alongside the wages and rewards of solidarity. It is a way of thinking that has shaped Shamasunder profoundly.
“You can keep your shirt clean and you can keep yourself feeling righteous from a distance,” he says, “But once you step into the muck of the world, you’re going to make mistakes and you’re going to get your shirt dirty. And both of you are going to be changed forever.”
-

UCSF Health Care Workers to Serve in Navajo Nation
A team of UC San Francisco health care workers is traveling to Arizona and New Mexico to begin a one month voluntary assignment providing urgently needed health care support for patients in the Navajo Nation
-

Dial Fellowship
Equipping remarkable social entrepreneurs with new communications tools to strengthen their voices and extend the impact of their work.
-
 Dial Fellows
Dial FellowsLessons from Rwanda for COVID-19
Dr. Agnes Binagwaho, Rwanda’s former Minister of Health, shares her experience rebuilding the country’s health care system and her insights on an equitable response to a pandemic.
Connected Stories
-
Beyond Recycling
How a digital marketplace for excess goods helps corporations, schools, and governments drastically reduce waste and save millions.
Dial Fellows -
Passing new laws isn’t enough. We also need to enforce the ones that already exist.
With Public Rights Project, Jill Habig is helping state, local and tribal governments enforce existing laws that protect jobs, housing, and rights for their communities.
Dial Fellows -

Who do we follow when we “follow the science”?
Immunologist Max Krummel has a bold vision for an inclusive, interdisciplinary future.
Dial Fellows